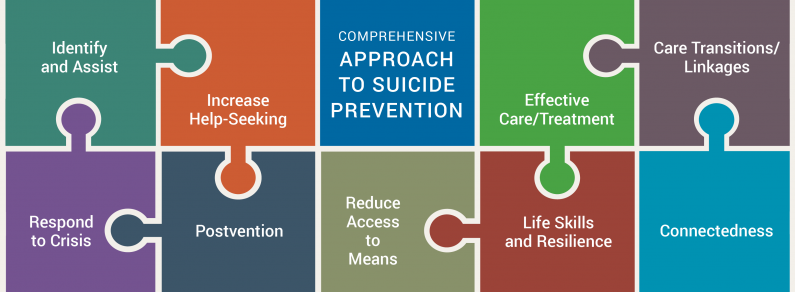
Effective suicide prevention is comprehensive: it requires a combination of efforts that work together to address different aspects of the problem.
The model above shows nine strategies that form a comprehensive approach to suicide prevention and mental health promotion. Each strategy is a broad goal that can be advanced through an array of possible activities (i.e., programs, policies, practices, and services). This model of a comprehensive approach was adapted from a model developed for campuses by SPRC and the Jed Foundation, drawing on the U.S. Air Force Suicide Prevention Program.
Identify and Assist Persons at Risk
Many people in distress don’t seek help or support on their own. Identifying people at risk for suicide can help you reach those in the greatest need and connect them to care and support. Examples of activities in this strategy include gatekeeper training, suicide screening, and teaching warning signs.
Increase Help-Seeking
By teaching people to recognize when they need support—and helping them to find it—you can enable them to reduce their suicide risk. Self-help tools and outreach campaigns are examples of ways to lower an individual’s barriers to obtaining help, such as not knowing what services exist or believing that help won’t be effective. Other interventions might address the social and structural environment by, for example, fostering peer norms that support help-seeking or making services more convenient and culturally appropriate.
Ensure Access to Effective Mental Health and Suicide Care and Treatment
A key element of suicide prevention is ensuring that individuals with suicide risk have timely access to evidence-based treatments, suicide prevention interventions, and coordinated systems of care. Suicide prevention interventions such as safety planning and evidence-based treatments and therapies delivered by trained providers can lead to significant improvement and recovery. SPRC encourages health and behavioral health care systems to adopt the Zero Suicide framework for integrating these approaches into their systems. Reducing financial, cultural, and logistical barriers to care is another important strategy for ensuring access to effective mental health and suicide care treatment.
Support Safe Care Transitions and Create Organizational Linkages
You can reduce patients’ suicide risk by ensuring that they have an uninterrupted transition of care and by facilitating the exchange of information among the various individuals and organizations that contribute to their care. Individuals at risk for suicide and their support networks (e.g., families) must also be part of the communication process. Tools and practices that support continuity of care include formal referral protocols, interagency agreements, cross-training, follow-up contacts, rapid referrals, and patient and family education.
Respond Effectively to Individuals in Crisis
Individuals in your school, organization, or community who are experiencing severe emotional distress may need a range of services. A full continuum of care includes not only hotlines and helplines but also mobile crisis teams, walk-in crisis clinics, hospital-based psychiatric emergency services, and peer-support programs. Crisis services directly address suicide risk by providing evaluation, stabilization, and referrals to ongoing care.
Provide for Immediate and Long-Term Postvention
A postvention plan is a set of protocols to help your organization or community respond effectively and compassionately to a suicide death. Immediate responses focus on supporting those affected by the suicide death and reducing risk to other vulnerable individuals. Postvention efforts should also include intermediate and long-term supports for people bereaved by suicide.
Reduce Access to Means of Suicide
One important way to reduce the risk of death by suicide is to prevent individuals in suicidal crisis from obtaining and using lethal methods of self-harm. Examples of actions to reduce access to lethal means include educating the families of those in crisis about safely storing medications and firearms, distributing gun safety locks, changing medication packaging, and installing barriers on bridges.
Enhance Life Skills and Resilience
By helping people build life skills, such as critical thinking, stress management, and coping, you can prepare them to safely address challenges such as economic stress, divorce, physical illness, and aging. Resilience—the ability to cope with adversity and adapt to change—is a protective factor against suicide risk. While it has some overlap with life skills, resilience also encompasses other attributes such as optimism, positive self-concept, and the ability to remain hopeful. Skills training, mobile apps, and self-help materials are examples of ways to increase life skills and build resilience.
Promote Social Connectedness and Support
Supportive relationships and community connectedness can help protect individuals against suicide despite the presence of risk factors in their lives. You can enhance connectedness through social programs for specific population groups (such as older adults or LGBT youth) and through other activities that reduce isolation, promote a sense of belonging, and foster emotionally supportive relationships.
Original Source: https://sprc.org/effective-prevention/comprehensive-approach